This fact-checked database helps journalists track how Nigeria tackles maternal mortality
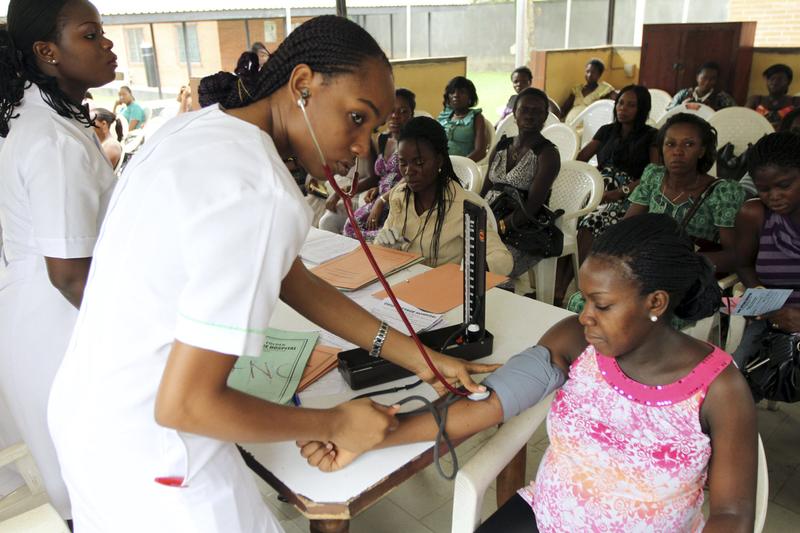
A nurse inspects a pregnant woman at a maternity hospital in Port Harcourt (Nigeria). REUTERS/Akintunde Akinleye
Maternal mortality is one of Nigeria’s most persistent health challenges. The country’s maternal mortality ratio is rated as very high by Unicef with 917 deaths per 100,000 live births recorded in 2017. Research suggests the country accounts for 20% of global maternal deaths. The rate has remained high for two decades despite efforts to address the issue by government and national and international initiatives.
To help reporters interrogate and cover maternal mortality and health, last year Nigerian journalist Ashley Okwuosa and engineer Chuma Asuzu launched the Maternal Figures project from Toronto, Canada. The duo has created a fact-checked database of 160 policy interventions that have been implemented to reduce maternal mortality in the country. The database serves both as a resource for journalists looking to produce in-depth reporting and a chance to investigate the impact of health interventions from a solutions journalism perspective.
By collecting and verifying information on maternal health programmes and initiatives, Maternal Figures also serves as an accountability check: many of the interventions in place are funded by local and international donors with little scrutiny on the impact of their efforts.
“We knew that maternal mortality was an endemic problem in Nigeria. Anyone that is Nigerian will know how commonplace it is despite how unfortunate a scenario it is,” says Okwuosa. “There were news reports on funding, including from large international organisations, going into programmes and training to hopefully reduce the rate at which women were dying, but a lot of reporting stopped there.”
For a country that still faces significant challenges to meet the Sustainable Development Goals, Okwuosa was left wondering what would happen when the next deadline comes around: “If Nigeria doesn’t meet its 2030 goals, will we have a better understanding of why that didn’t happen?”

Building the database
To build the database, Okwuosa and Asuzu gathered information from news reports, policy documents and registries on government websites. They worked with local public health organisations, made FOI requests and spent time in Nigeria gathering and verifying information as well as working remotely and cold-calling and emailing foundations, donors and organisations behind maternal health programmes.
There are at least 350 interventions in addition to the 160 in the public database waiting to be fact-checked. Interventions specific to states, a local government area, community or national in scope all feature in the database. Those included must aim to reduce maternal mortality and show long-term investment in the country or community in some form.
The team also ran surveys of mothers and separately journalists in Nigeria to find out what programmes had been successful and what information the news media would need to strengthen reporting on maternal health. The database and its function are designed around journalists’ needs, says Asuzu.
Supporting journalists
Stories produced with Maternal Figures’ help so far include reporting on the use of traditional birth attendants and where this practice was potentially endangering women and where it had been revamped to better work alongside clinical care. As the reporter’s state was banning the practice, she looked at what could be learnt from other regions where progress had been made.
The initiative is now offering reporting fellowships to journalists looking to report on maternal health in Nigeria or introduce solutions journalism to their newsrooms. The team hopes these grants will encourage more reporting on maternal health through a solutions lens particularly in places where there is greater need for maternal health provision and where interventions have gone unreported or been less subject to scrutiny.
An example: there’s a government revitalisation programme in Niger state that’s intended to revamp hospitals. “It involves a lot of money and is co-partnered between the Nigerian government and a development organisation, but there’s been very little reporting since the memorandum of understanding was signed,” says Okwuosa. “It exists in a state where there is an incredible need for maternal healthcare and healthcare in general.”
Premium Times reporter Chiamaka Okafor applied to the Maternal Figures fellowship to expand from reporting on news, politics and gender to additionally covering health. She used the grant to report on the role of malaria in maternal deaths in Nigeria and interrogated the Nigerian government’s National Malaria Strategic Plan 2014-2020, which promised to eliminate the disease in the country, and its implementation in the context of maternal health.
Her reporting helped add extra information about this intervention and its application in three very different areas to the Maternal Figures database. As more stories are reported and interventions returned to by journalists, the team hopes that a multi-layered understanding of maternal health in Nigeria will be built.
Business Day reporter Desmond Okon used the fellowship to report on a maternal health intervention helping women in Benue State in the North Central region of Nigeria.
“The maternal mortality rate is a burden in Nigeria and the extensive and in-depth reporting that Maternal Figures now promotes could expose the realities of maternal mortality in Nigeria and help map solutions that specifically address how it affects communities,” he says, adding that applying for the fellowship allowed him “to be a part of something” and open potential career opportunities.
Reporting on health in Nigeria
The fellowship also helped secure Okon’s first reporting trip outside of Lagos. This hints at a challenge for health reporting in Nigeria: health, including maternal health, needs and provisions in rural communities are very different from the ones in urban centres. But with many newsrooms based in cities, reporters may not be sent out to report from more remote communities.
The reliability of and access to health data is also an issue. The initial pitch for the project was to look at how interventions had affected maternal mortality figures, but the team couldn’t get consistent data for the past 30 years so had to abandon the idea. With maternal mortality data collected by several different bodies (from the World Bank and WHO to national bodies) the numbers are often different and ascertaining which count is most accurate is difficult, says Asuzu. Maternal Figures hopes to contribute to a better data collection process over time.
“Every Nigerian journalist has a tale about the limitations that a lack of access and data can bring to your work,” says Okon, who hopes that the reporting supported by Maternal Figures’ database and fellowships programme will provide new data on maternal mortality rates. Okafor found no specific data on malaria in pregnancy in Nigeria, for example, despite the high burden of the disease in the country. For her story, she had to use data for malaria in under-fives, get information from hospital reports and use “deduction by proxy” to build a dataset.
The project encourages others to submit interventions for review reflecting its openness and its commitment to strengthening understanding and reporting on maternal health through collaboration.
Talking to public health experts helped shape the project’s initial plans and partnering with Code for Africa provided experience of developing digital solutions for journalists potentially working with low data or internet connectivity. Its initial consultations with journalists in the design process have also continued and the team regularly speaks with newsrooms and runs newsroom training sessions. It’s also developed a course Reporting on Endemic Problems with Solutions Journalism.
The team has been invited into Nigerian newsrooms and is keen to offer training and continue “a large conversation about how to report on health in Nigeria”, says Okwuosa: “We want to learn how other people are wading through the accountability issue, getting people to talk to them, getting people to share certain information.”
Planning ahead
The Maternal Figures team have ambitious goals for the project. “We have plans to scale. This is a model that lends itself to another country,” says Okwuosa. India would be a natural choice owing to a high maternal mortality rate in the country. More funding for journalists and on-the-ground fact-checking are priorities.
“We see Maternal Figures as a 10-year project to 2030 and the SDGs, and we’re looking for funding partners,” says Asuzu. Both manage the project alongside other work commitments and have been “creative” in raising funding, applying individually for fellowships and programmes to secure support. Initial funding came from the Brown Institute. Support from the Solutions Journalism Network has been crucial too.
Funding from journalistic institutions makes sense as opposed to seeking support from development organisations, says Okwuosa: “If a reporter wants to write about an organisation and we were getting money from them it can get murky. Journalistic institutions understand the need for us to be independent.”
For reporters in Nigeria, Maternal Figures hopes to provide the funding and space to report on an issue that is often dismissed as commonplace, says Okwuosa. Okafor sees the potential: “Stories relating to pregnancy are inexhaustible and the data in Maternal Figures is untapped. We are not paying enough attention to women’s health. Covering women’s bodies and experience from an educational perspective is important – it’s what the media can do to better inform its audience about their health.”
Laura Oliver is a freelance journalist based in the UK. She has written for the 'Guardian', BBC, 'The Week' and more. She is a visiting lecturer in online journalism at City, University of London, and works as an audience strategy consultant for newsrooms. You can find her work here.







